|
Associate Professor Vimol Srisukh, Department of Food Chemistry, Faculty of Pharmacy, Mahidol University. |
|
| 196,479 View 1 days ago | |
| Publication date: 2014-04-06 |
What is AMD?
The retina is the innermost area of the eye. When we look at an object, the light which strikes the object is reflected and passes through the eye and finally strikes the retina. The retina will then convert the light energy into nerve impulses which are transmitted to the brain by the optic nerve where they are interpreted as sight. The focal center of the retina, an area called the macula lutea, posses the highest concentration of photoreceptors and is responsible for central vision and high-resolution acuity. If the macula lutea is destroyed, vision will be blurred.
Age-related macular degeneration (AMD) is the disease that specifically targeting the macula lutea. It gradually destroys the macula. In some people, AMD advances so slowly that vision loss does not occur for a long time. In others, the disorder progresses faster and may lead to a loss of vision in one or both eyes. It is the principal cause of blindness among people aged 65 years and older in the western world.
Are there many types of AMD?
According to the National Eye Institute (NEI) of the National Institute of Health (NIH), AMD is classified by severity into 2 types:
- Early (or dry) AMD. It is the most common form of AMD in its early or intermediate stages. It occurs in about 90 percent of the people with the condition. Dry AMD happens when the light-sensitive cells in the macula slowly break down, gradually blurring central vision in the affected eye. As dry AMD progresses, you may see a blurred spot in the center of your vision.
- Late (or wet) AMD. Wet AMD affects about 10 percent of all people with AMD. Wet AMD happens when abnormal blood vessels behind the retina start to grow under the macula. These new blood vessels can be fragile and leak blood and fluid. The blood and fluid cause the macula to swell and damage occurs rapidly. The damage may also cause scarring of the retina.
During the early stages of wet AMD straight lines may appear wavy. People with wet AMD also may develop a blurred spot, which results in loss of central vision. What are the risk factors of AMD?
A variety of factors contribute to an increased risk of AMD, including age, cigarette smoking, light iris coloration, sunlight exposure, poor nutritional status, and genetics. Women also exhibit a higher incidence of AMD than men.
Does the human body contain any defense mechanisms to prevent the damage of the retina?
Let's follow the light path after it enters the eye. When light passes into the eye through the cornea and the lens, the cornea has the capacity to screen some of the ultraviolet (UV) light from entering the eye. The light is then focused by the lens onto the retina. Among the visible light striking the retina, high-energy, blue wavelengths of visible light are 100 times more effective at inducing free radical formation in the cells of the retina than the low-energy, red wavelength of visible light. The focal center of the retina, the macula lutea, contains a high concentration of macular pigment that is composed of lutein and zeaxanthin. These two xanthophylls are believed to function as antioxidants to protect the photoreceptor cells from the potential damage caused by free radicals that can be generated in these cells by the oxygen tension and exposure to light. In addition, both lutein and zeaxanthin are also believed to be responsible for filtering the high-energy wavelengths of blue light. It is estimated that the reduction in blue light reaching the macula, typically a 40% reduction, could significantly reduce the oxidative stress on the retina.
What should you eat to delay AMD?
Lutein and zeaxanthin are non-provitamin A carotenoids which means that they cannot be transformed into vitamin A after the ingestion. They are grouped as Xanthophyll carotenoids. Humans do not have the capacity to synthesize lutein and zeaxanthin in their bodies, therefore depend entirely on dietary sources of these compounds. Lutein and zeaxanthin are the only two carotenoids which are present at the macula and the lens.
Results from 12 epidemiological studies (studies among large groups of population) that evaluated the relationship between dietary intake and/or blood levels of xanthophyll carotenoids and AMD were not consistent. But most of the studies found that consumptions of diets with the highest lutein and zeaxanthin or the highest level of serum lutein and zeaxanthin are associated with the lowest risk for AMD (compared with the lowest lutein and zeaxanthin group). Furthermore, reports from 7 clinical studies (human studies) have shown that the intake of lutein and zeaxanthin resulted in a significant increase in lutein levels in the blood and in macular pigment optical density and an improvement in visual acuity regardless of whether the dietary source of lutein and zeaxanthin ingested was from foods or dietary supplements. The overall picture suggests that a diet high in lutein and zeaxanthin has a potential protective role against AMD.
Since lutein and zeaxanthin are compounds that belong to the carotenoid group, they can be found in a wide variety of fruits and vegetables, especially in dark-green leafy vegetables such as kale (4.8-13.4 milligram of lutein/100 gram of fresh weight) and spinach (6.5-13.0 milligram of lutein/100 gram of fresh weight). Although eggs are not the richest source of lutein and zeaxanthin, they are considered a good source due to their high availability. So people who used to avoid consumptions of eggs might want to reconsider. Currently, no recommendation is set for the daily intake of lutein and zeaxanthin. Doses reported in the studies include 2.5-30 mg of lutein/day and 0.4-2 mg of zeaxanthin/day. Studies on visual acuity in AMD patients were reported, using diets containing 150 gram of spinach (approximately 14 mg of lutein) or supplements containing lutein and zeaxanthin 4-7 times per week for up to 1 year, 10 mg of lutein plus antioxidant supplement daily, 10 mg of lutein and 1 mg of zeaxanthin daily, etc.
In conclusion, the role of lutein and zeaxanthin in the human eye is not completely understood besides the absorption of blue light and the antioxidant activity. In addition, the clinical studies were conducted in small groups and results have not been entirely consistent. Nevertheless, consumption of lutein and zeaxanthin in the form of vegetables or other foods is quite harmless. The following table shows lutein/zeaxanthin contents in several green vegetables and other foods. The most familiar ones are kale and spinach; both vegetables contain high levels of lutein.
Now it should dawn on you why the lawyer character, Louis Litt, in the popular cable TV series “Suits”, was so obsessed with the kale & spinach smoothie drink to the point that he prepared it himself in the kitchenette of the law firm. 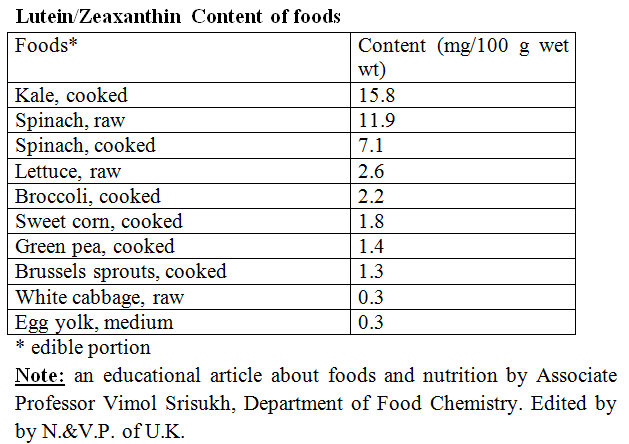
Reference
- Bahrami H, Melia M, Dagnelie G. Lutein supplementation in retinitis pigmentosa: PC-based vision assessment in a randomized double-masked, placebo-controlled clinical trial (NCT00029289). BMC Ophthalmol 2006;6:23.
- Beatty S, Boulton M, Henson D, Koh H, Murray I. Macular pigment and age-related macular degeneration. Br J Ophthalmol 1999;83:867-77.
- Beatty S, Nolan J, Kavanagh H, O’Donovan. Macular pigment optical density and its relationship with serum and dietary levels of lutein and zeaxanthin. Arch Biochem Biophys 2004;430:70-6.
- Berenschot T, Goldbohm R, Klopping W, et al. Influence of lutein supplementation on macular pigment, assessed with two objective techniques. Invest Ophthalmol Vis Sci 2000;41:3322-6.
- Evans JA, Johnson EJ. Something new under the sun: lutein’s role in skin health. Am J Lifestyle Med 2009;3:349.
- Goldberg J, Flowerdew G, Smith E, Brody J, Tso M. Factors associated with age-related macular degeneration. An analysis of data from the first National Health and Nutritional Examination Survey. Am J Epidemiol 1988;128:700-10.
- Hammond Jr B, Johnson E, Russell R, et al. Dietary modification of human pigment density. Invest Ophthalmol Vis Sci 2000;41:3322-6.
- Handelman GJ, Ninghtingale ZD, Lichtenstein AH, Schaefer EJ, Blumberg JB. Lutein and zeaxanthin concentrations in plasma after dietary supplementation with egg yolk. Am J Clin Nutr 1999;70:247-51.
- Johnson E, Hammond Jr B, Yeum K, et al. Relation among serum and tissue concentrations of lutein and zeaxanthin and macular pigment density. Am J Clin Nutr 2000; 71:1555-62.
- Klaver C, Wolfs R, Vingerling J, Hofman J, de Jong P. Age-specific prevalence and causes of blindness and visual impairment in an older population: the Rotterdam Study. Arch Ophthalmol 1998;116:653-8.
- Koh H, Murray I, Nolan D, Carden D, Feather J, Beatty S. Plasma and macular responses to lutein supplement in subjects with and without age-related maculopathy: a pilot study. Exp Eye Res 2004;79:21-7.
- Kopsell DA, Kopsell DE, Curran-Celentano J, Wenzel AJ. Genetic variability for lutein concentrations in leafy vegetable crops can influence serum carotenoid levels and macular pigment optical density in human subjects. ISHS Acta Horticulture 841: II International Symposium on Human Health Effects of Fruits and Vegetables: FAVHEALTH 2007.
- Kvansakul J, Rodriguez-Carmona M, Edgar D, et al. Supplementation with the carotenoid lutein or zeaxanthin improves human visual performance. Ophthalmic Physiol Opt 2006;26:362-71.
- Landrum J. Serum and macular pigment response to 2.4 mg dosage of lutein. ARVO 2000;2000:41.
- Landrum J, Bone R, Joa H, Kilburn M, Moore L, Sprague K. A one year study of the macular pigment: the effect of 140 days of a lutein
- Mangels AR, Holden JM, Beecher GR, Forman MR, Lanza E. Carotenoid content of fruits and vegetables: an evaluation of analytic data. J Am Diet Assoc 1993;93:284-96.
- Massacessi A, Faletra R, Gerosa G, Staurenghi G, Orzalesi N. The effect of oral supplementation of macular carotenoids (lutain and zeaxanthin) on the prevention of age-related macular degeneration: an 18-month follow-up study. ARVO 2001;42:S234.
- Moeller S, Parekh N, Tinker L, et al. Associations between intermediate age-related macular degeneration and lutein and zeaxanthin in the Carotenoids in Age-related Eye Disease Study (CAREDS): ancillary study of the Women’s Health Initiative. Arch Ophthalmol 2006;124:1151-62.
- Nolan J, Stack J, Lellerio J, et al. Monthly consistency of macular pigment optical density and serum concentrations of lutein and zeaxanthin. Curr Eye Res 2006;31:199-213.
- Richer S. ARMD-pilot (case series) environmental intervention data. J AM OPTOM ASSOC 1999;70:24-36.
- Richer S, Stiles W, Statkute L, et al. Double-masked, placebo-controlled, randomized trial of lutein and antioxidant supplementation in the intervention of atopic age-related macular degeneration: the Veterans LAST study (Lutein Antioxidant Supplementation Trial). Optometry 2004;75:216-30.
- Roberts RL, Green J, Lewis B. Lutein and zeaxanthin in eye and skin health. Clin Dermatol 2009;27:195-201.
- Seddon J, Anani A, Sperduto R, et al. Dietary carotenoids, vitamin A, C, E and advanced age-related macular degeneration. Eye Disease Case Controlled Study Group. JAMA 1994;272:1413-20.
- Sommerburg O, Keunen J, Bird A, van Kuijk F. Fruits and vegetables that are sources of lutain and zeaxanthin: the macular pigment in human eyes. Br J Ophthalmol 1998;82:907-10.
- Surai PF, MacpPherson A, Speake BK, Sparks NH. Designer egg evaluation in a controlled trial. Eur J Clin Nutr 2005;54:298-305.
Recommended articles

|
Young Coconut Water: The functional drink from nature 10 minutes ago |

|
STOP SMOKING with Nicotine Replacement Therapy 12 minutes ago |

|
Thai Traditional Medicine Theory in Relation to Seasons Part 2 15 minutes ago |

|
Thai Traditional Medicine Theory in Relation to Seasons Part 1 15 minutes ago |

|
Top 10 Selenium-Rich Foods & Health Benefit 2 hours ago |

|
As a Diabetic, What are my Choices for Alternative Sweeteners? 3 hours ago |

|
Food allergy in children:a brief information for new parents 3 hours ago |

|
Drugs that should be avoided in patients with dementia 4 hours ago |
|
|
Preservatives in sausages, ham, and bologna 4 hours ago |

|
Melatonin in foods 6 hours ago |
